Nationwide shutdowns with no end in sight.
Images of refrigerated trucks converted into temporary morgues.
Harrowing testimonies from frontline workers.
At the beginning of the COVID-19 pandemic, people were scared. But while most stayed home, health care providers showed up every day and worked tirelessly to provide their patients with the best care possible.
However, many patients requiring routine screenings and procedures continued avoiding hospitals and doctor’s offices even as these facilities followed the highest infection control standards. This phenomenon led to a medical backlog, which has had lasting impacts, including delays in early detection of different cancers, increased death rate from heart attacks and strokes, and surgical backlog.
Despite reassurance from experts, fear and uncertainty kept many patients away from medical facilities.
Ranju Gupta, an oncologist specializing in breast cancer at Lehigh Valley Health Network, noticed her patients were skipping appointments earlier this year.
“We definitely saw patients skipping or trying to postpone, especially older patients,” Gupta said.
This effect was not exclusive to oncology. Nicolas Hernandez, a family medicine physician with the Northwell Health system, also noticed patients canceling and postponing appointments. He attributed these fears to the lack of knowledge about the pandemic at the time.
“There were still a lot of unknowns about how the virus transmitted, how to go about treating it, how to go about detecting it, so those limitations really created a lot of chaos,” Hernandez said.
This backlog doesn’t come without consequences. According to an article published in The Lancet, a peer-reviewed medical journal, experts predict a 7.9 to 9.6 percent increase in breast cancer deaths, and a 15.3 to 16.6 percent increase in colorectal cancer deaths in the next five years due to the diagnostic delays the pandemic has caused.
Gupta worries about her patients skipping mammograms, as early detection is the key to a good prognosis when it comes to treatment for breast cancer, she said.
Although not every advanced stage cancer diagnosis can be attributed to COVID-19 backlog, Gupta said delays in diagnosis can lead to worse outcomes in her field.
In addition to concerns about breast cancer patients, doctors are worried about the pandemic’s impact on colon cancer. With patients delaying colonoscopies, some colon cancer diagnoses are being delayed as well.
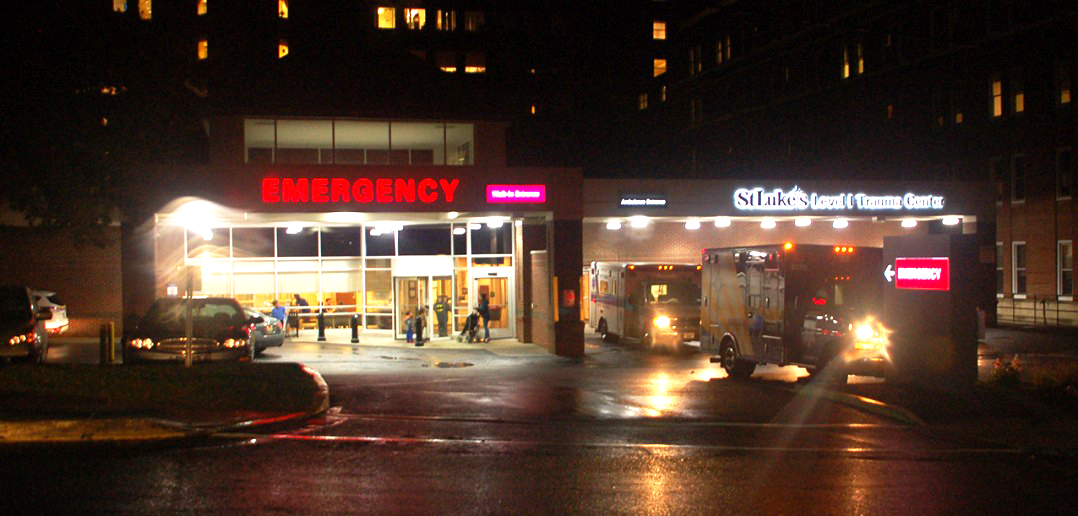
John Sojka, a fourth-year general surgery resident at St. Luke’s Hospital, said many of his colleagues in colorectal surgery are concerned.
When colon cancer is caught early, it can be cured with surgery, Sojka said. Although this cancer takes years to progress, when it gets to the advanced stage, the prognosis is poorer, he added.
Hernandez also said that patients delaying colonoscopies can face significant consequences.
“A lot of older folks who end up having some of these incidental findings, unfortunately don’t do well,” Hernandez said. “We’ve seen a lot of colon cancer, it’s a slow brewing cancer, but it gets to the point where you can’t really correct it.”
Oncology isn’t the only area of concern for experts. Another issue some doctors have noticed is that some people are delaying treatment for medical emergencies, like heart attacks or strokes.
Gupta said that at the height of the pandemic, people were suffering cardiac events and not coming to the hospital until very late.
“People with chest pain or heart attacks were not going to the hospital because they were like ‘OK, this is a COVID hospital, so if I went to the hospital I will get COVID’,” Gupta said. “And what happened was there was high mortality, people died of heart attacks and congestive heart failures because they did not go to the hospital in a timely fashion.”
These life-threatening emergencies, though unrelated to the pandemic, were still made a priority by health care workers. However, their time and resources had to be reallocated in some way to accommodate the influx of COVID-19 patients. As a result, elective surgeries were postponed.
According to an article by consulting firm McKinsey and Company, hospitals across the nation have seen an average of about a 35 percent decrease in operating room volumes from March through July 2020, with a peak of 59 percent decrease in April.
Sojka said St. Luke’s volume of surgical procedures was cut at half in the beginning of the pandemic when elective surgeries were postponed. He believes taking this step was the right thing to do.
“It was good for everybody. I think that the patients wanted to put off getting their elective surgical procedures, as well as health care providers didn’t want people to come into the hospital for potential exposures to COVID-19 when they are getting something done that may not necessarily be needed right away,” Sojka said.
Although postponing elective surgeries was a necessary step, it left hospitals with a backlog to catch up on when COVID-19 cases declined.
Nicole Adler, Associate Chief Medical Officer at NYU Langone Hospital – Long Island, said her hospital also had to postpone elective surgeries in March and April as well, but they have since caught up on the backlog.
“We’ve been really fortunate to be able to schedule patients for procedures, and I think we’ve been able to get patients the care that they need,” she said.
Adler attributes patients’ willingness to come back for procedures, even elective ones, to NYU Langone’s high standards for safety precautions. These include separate designated COVID-19 units, strict social distancing measures and mask requirements, as well as robust virtual care programs.
“A lot has changed since March and April, we did a lot of learning during and after that time and tried to understand what were opportunities for us, so that we could make sure that should there be another influx of patients, we could really strive to make sure that we were providing even better care for our patients,” Adler said.
Gupta also said health care has come a long way since March, with her office taking precautions as well to ensure the safest patient experience.
Gupta said hospitals may be even safer than most public places due to their diligent infection control standards, and she encourages patients not to fear them. She has no plans to put off her own screenings amid the pandemic.
“I have my mammography coming up in December. I will be going,” Gupta said.
Despite these precautions, some patients are still apprehensive about entering a medical facility. Hernandez believes the key to alleviating these concerns is education and communication between providers and their patients.
“Every day we are getting more and more information,” Hernandez said. “We’re understanding what that information means and we’re learning how to manage it.”



Comment Policy
Comments posted to The Brown and White website are reviewed by a moderator before being approved. Incendiary speech or harassing language, including comments targeted at individuals, may be deemed unacceptable and not published. Spam and other soliciting will also be declined.
The Brown and White also reserves the right to refuse the publication of entirely anonymous comments.